Effect of Teaching
on Hospital Productivity
S. Grosskopf
Economics
Southern Illinois University
Carbondale, IL 62901-4515
D. Margaritis
Economics
Waikato University
Hamilton, New Zealand
V. Valdmanis
Health Administration Policy
University of Oklahoma
Box 26901
Oklahoma City, OK 73190
Effect of Teaching on Hospital Productivity
S. Grosskopf, D. Margaritis, V. Valdmanis*
Introduction
One of the interesting features of hospitals is their multiproduct capability. In addition to providing various types of direct patient care, some hospitals also offer training opportunities for medical students and physicians-in-training (i.e., residents). One consequence of these additional responsibilities is that costs typically are higher in teaching hospitals than in their non-teaching counterparts.
The goal of this paper is to determine the impact teaching programs have on hospital productivity. The technique we use is a nonparametric frontier approach (also known as DEA -- data envelopment analysis). One advantage of this approach over other empirical studies in this area is that we infer the real resource costs of residents from the underlying production technology, in contrast to the accounting approaches that have been used elsewhere.
In order to assess relative productivity, a reference technology or "best practice frontier" is constructed from the observations in our sample under assumptions of both strong and weak disposability of inputs. By analyzing medical residents as weakly disposable inputs, we can estimate their opportunity cost in terms of foregone medical services, or reduced hospital productivity. In the next section, we discuss the previous empirical work analyzing teaching costs on hospitals. In section III we describe our methodology. The fourth section contains the data and results. Section IV concludes the paper.
__________________
The authors are listed alphabetically.
II. Background
Early analysis of the effect of teaching on hospital cost focused on how residents affected service levels. For example, Sloan et al. (1983) argued that simply determining overall cost differentials was not helpful for policy purposes; rather, the impact that teaching had on other hospital services, for example nursing services, was relevant. Further, these authors argued that it was crucial that we understand the true nature of the costs of teaching, both direct and indirect, especially when reimbursements are higher for teaching hospitals. Lee and Hadley (1985) followed this general line of inquiry and analyzed the impact of residents, specifically as inputs, on the provision of hospital services. They point out that if residents are "inferior" factors of production, a reduction in the demand for hospital services will lead to an increase in demand for these inputs. On the other hand, if price competition increases in the hospital sector, the demand for residents will also be reduced because of a reduced demand for the more costly teaching hospitals.
Cameron (1985) also assessed the direct and indirect costs of teaching. Higher indirect costs were identified as increased use of ancillary services and/or increased lengths of stay as well as the overhead allocated to the medical education cost center. Direct costs include salaries and fringe benefits of the residents plus the costs attributed to teaching activities such as supervisory time. Determining the cost of medical education is confounded in that medical education is carried on in conjunction with patient care. In other words, medical education and patient care are jointly produced (Cameron, 1985). By assessing characteristics that also affect hospital costs such as patient case mix and holding these factors constant, Cameron found that university teaching hospitals were 33% more costly than non-teaching hospitals. Major teaching hospitals and minor teaching hospitals were 18% and 9% more costly relative to non-teaching hospitals, respectively. These findings indicate that teaching adds costs to hospital care that are over and above the severity of their patient load. This result was verified by Rich et al. (1990) who found that teaching hospitals cost 9% to 30% more than non-teaching hospitals and attributed the cost differential to increased volume of services per patient. The increased services were attributed to inexperienced residents who tend to overprescribe testing.
The relation between experience and hospital charges was directly addressed by Rich et al. (1991) -- a statistically negative relationship was found to exist between resident experience and hospital charges. Hence cost differentials may vary depending on the median experience of the resident staff. This information could prove useful in designing prospective payment systems (PPS) with built in allowances for teaching.
The teaching aspects of hospital care are also evident by comparing the treatment plans of resident physicians vis-<-vis attending physicians (physicians who have finished their post-graduate training). More experienced physicians directly caring for their own private patients in non-teaching community hospitals are typically more aware of their patients' conditions and this may be reflected by more efficient care, i.e., fewer diagnostic tests. This dynamic may in part explain why operating costs in teaching hospitals are higher, i.e., inexperienced residents may inefficiently use hospital resources (Feinglass et al., 1991). However, it was also found that physicians who gave residents autonomy were also lower cost providers themselves, indicating that tradeoffs between these two physician types exist and there may be efficiencies gained by using the lower priced resident physician (Feinglass, 1991).
In other words, it may be argued that since residents may be utilized as substitutes for physicians, at least a portion of teaching costs may be offset by lower physician input costs (Campbell, et al., 1991). The extent of this substitution, however, would depend on the degree to which staff physicians are paid for directly by the hospital. Campbell, et al. (1991) studied teaching versus non-teaching hospitals in the Veteran's Administration (VA) system, and found that the financial performance was indistinguishable between the two hospital types.
Rogowski and Newhouse (1992) expanded on previous work to incorporate the multi-dimensionality of hospital outputs and the hospitals' commitments to teaching by using a spline function where the spline was dummy coded as teaching intensity. Based on this approach, these authors were able to ascertain whether teaching programs were being under-or overpaid. In the pre-PPS period, Medicare reimbursed hospitals for their teaching commitment on the basis of allowable costs which included the direct costs as well as the indirect costs defined above (Rossman and Marcus, 1991). Since the introduction of PPS, payment has been altered to reimburse on an average cost basis. In assessing this new reimbursement method, Rogowski and Newhouse (1992) found that smaller and larger teaching programs were being overpaid by Medicare reimbursement for teaching costs whereas medium-sized teaching programs were being underpaid. Their results suggest that using a PPS approach based on accounting data may bias the payment for residents.
With the exception of results for VA
hospitals, the general consensus is that teaching activities add
to hospital costs. However, given the difficulties of singling
out teaching from other hospital services based on accounting
data, we suggest an alternative approach to determining the impact
of resident on hospital costs. This approach is described below.
III. Methodology
The approach used in this paper was introduced by Farrell (1957) and expanded by Charnes, Cooper, and Rhodes (1978) and F@re, Grosskopf, and Lovell (1985, 1994) and is commonly referred to as data envelopment analysis (DEA). This method is both non-parametric and deterministic. The best practice frontier is derived from all the observations in the sample and is constructed from the observed inputs and outputs by linear programming techniques. The efficiency of each observation is determined relative to the best practice frontier, providing a relative measure of efficiency rather than an absolute measure of efficiency.
The nonparametric approach we employ provides a great deal of flexibility in modeling technology. Other advantages include the fact that it does not require specification of a functional form, it readily models joint outputs, and it does not require data on input prices or costs.
The flexibility in terms of modeling the underlying technology is what we exploit to determine possible opportunity costs of residents in teaching hospitals. In particular, we allow for the possibility that after some point, additional residents may not result in increased hospital (nonteaching) outputs. This is achieved by allowing for the possibility of "congestion" by residents. We do this by varying the input disposability restrictions in the reference technology.
The reference technology is specified as a series of inequalities which construct the (best practice) frontier of technology as piecewise linear segments formed from the data. Suppose we have k = 1,...,K observations on hospitals in our sample. These hospitals produce m = 1,...,M outputs yk = (yk1,...,ykM) from n = 1,...,N inputs xk = (xk1,...,xkN). All input and output data are nonnegative.
We form the technology L(y,S) = {x: x can produce y} which satisfies strong disposability of inputs and outputs as
(1) 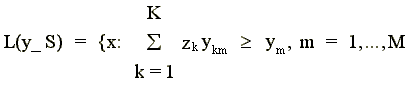
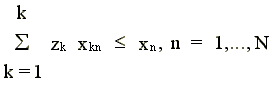
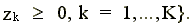
The technology is constructed as convex combinations of the data--the z's (the intensity variables) serve this purpose. For a more detailed discussion of how the reference technology is constructed, see, for example, Grosskopf (1986) or F@re, Grosskopf and Lovell (1994).
The technology, L(y,S),
by construction, does not allow for congesting effects of residents,
since strong disposability of inputs is imposed through the inequality
in the input constraints. To construct a technology which allows
for congestion effects of residents, we need to allow for weak
disposability of some inputs. This means that increases in the
these inputs may actually decrease output, i.e., they congest
production. This technology L(y,w)
is
(2) 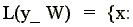
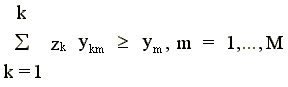
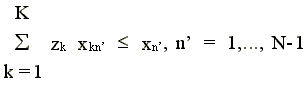
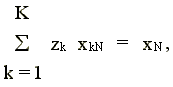
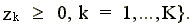
The technology in (2) allows for strong disposability of all inputs except the last input (N). Input N (residents in our case) is weakly disposable, which is imposed through the strict equality in the Nth input constraint.
These two technologies are illustrated
in Figure 1.
Figure 1: 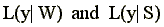
The isoquant UU is the best practice frontier for firms A, B, C, and D. Note that both firms A and B lie on the isoquant and therefore they are considered "efficient." Firm C lies interior to the isoquant and is considered inefficient by the amount OB/OC. Firm D lies on the isoquant but on the backward bending portion, where marginal product is negative. This implies that input x1 is congesting output in Firm D's production process and that decreasing the amount of x1 that Firm D uses would actually increase output.
We compute the efficiency of each hospital by solving the following linear programming problems:
(3) Fi(y,x,S) = min {8 : 8x 0 L(y,S)}
(4) Fi(y,x,W) = min {2: 2x 0 L(y,W)}.
In each case, we use the piecewise linear technologies specified in (1) and (2) as the constraints in the problem. The solutions to these problems tell us the factor by which inputs would have to be radially contracted to bring them to the frontier of technology, thus these values are less than or equal to one, with a value of one signaling efficiency. If we subtract this value from one we have the percent by which inputs could be reduced and still produce their current level of outputs.
If we take the ratio of these two values, we have a measure of the degree to which residents congest output:
(5) 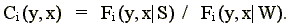
We apply this approach to a sample of
hospitals operating in the U.S. in order to determine whether
residents congest the production process of patient care. A description
of the data and results are given in the next section.
IV. Data and Results
The data used for this study is from the 1989 American Hospital Association (AHA) Survey of Hospitals. Our sample consists of 533 teaching hospitals which included hospitals that had non-zero values for all inputs and outputs and trained full time equivalent (FTE) medical residents/interns. As stated earlier, the DEA approach allows us to use multiple inputs and outputs in determining the best practice production frontier. In this analysis we use the following outputs and inputs. Outputs are defined as the total number of acute care patient days (Acute); total number of intensive care inpatient days (ICU); total number of subacute care days (Sub-acute); total number of surgeries (SURG); total number of outpatient and emergency room visits (Outpat), and total number of discharges (Discharges). We include both discharges and patient days as outputs in order to account for both "hotel" and medical outputs B la Granneman et al. (1987).
Inputs are defined as number of physicians with staffing privileges (Medstaff); number of FTE medical residents/interns (Medres); number of FTE registered nurses (RNs); number of FTE licensed/vocational nurses (LPNs); number of FTE other hospital personnel (FTEother); and number of licensed and staffed beds (BEDs). By directly adding physicians with staff privileges we overcome some of the shortcoming of omitting physicians which have troubled other studies (Campbell, et al., 1991). Descriptive statistics of outputs and inputs are given in Table 1. It should also be noted that in the literature, medical residents have been treated as both inputs and outputs in the joint production of hospital goods and services in the teaching hospital. In this paper, we treat medical residents solely as inputs. Since our outputs are restricted to medical care (and don't explicitly include a measure of teaching output), our measures of congestion capture the effects of residents on medical care only.
Our efficiency results are given in
Table 2. On average, the teaching hospitals in our sample had
an efficiency score of .90 under the assumption of strong disposability
of inputs and an efficiency score of .91 under the assumption
of weak disposability of inputs. Based on a simple t-test, we
cannot reject the hypothesis that the means are equal (t = -1.33,
p-value = 0.18 for a two-sided test). For the one-sided test
(Ho: Fi(y, x,S)
< Fi(y, x,W))
the p-value is 0.09, i.e., we accept at 5% but reject at 10%.
Using a non-parametric Mann-Whitney test for differences in medians,
the p-value = 0.049 for the one-sided test, i.e., we marginally
reject the null of equal medians even at the 5% level.
Table 1: Descriptive Statistics
Std.
Outputs Mean Deviation Min
Max
Acute 83273.26 58326.77 23.00 371531.00
ICU 14750.84 14471.84 224.00 206015.00
Subacute 20498.23 24658.10 65.00 270777.00
SURG 10369.51 7207.92 642.00 71659.00
OutPat 15772.90 131736.56 4052.00 937993.00
Discharges 15718.52 9007.42 1159.00
77373.00
Inputs
Medstaff 344.78 268.53 18.00 2076.00
MedRes 89.64 119.46 1.00 700.00
Rns 368.32 288.95 17.00 1741.00
LPNs 60.31 59.13 1.00 532.00
FTEother 1197.41 879.71 70.00 6676.00
BEDS 443.29 240.13 47.00 1479.00
Table 2: Efficiency Results
Std.
Efficiency Score Mean Dev. Min Max
Fi(y,xKS) .90 .103 .51 1.00
Fi(y,xKW)
.91 .102 .51 1.00
Statistical Tests
Ho: Fi(y,xKS) = Fi(y,xKW)
HA: Fi(y,xKS)
< Fi(y,xKW)
Means p = 0.09
(t-test)
Median p = 0.049
(Mann Whitney)
Table 3: Selective Statistics on Teaching Hospitals with and without Congestion
Variable N Median
Mean Std. Dev.
Ci(y,x) = 1 382 1.000 1.000 0.000
Ci(y,x) < 1 151 0.989 0.968 0.047
Resbeds1 382 0.069 0.114 0.145
Resbeds2 151 0.289 0.341 0.214
Resdocs1 382 0.115 0.175 0.229
Resdocs2 151 0.336 0.429 0.093
Ci(y,x) 533 1.000 0.991 0.029
Resbeds 533 0.110 0.178 0.198
Resdocs 533 0.157 0.247 0.274
We also wanted to ascertain if any differences exist between teaching hospitals that exhibit congestion from those hospitals that do not exhibit congestion. In Table 3, we present selective statistics for all hospitals in our sample and between teaching hospitals that have congesting factors versus hospitals that do not have congesting factors. These variables include a ratio of strongly disposable efficiency to weakly disposable efficiency, Ci(y,x), the ratio of residents to number of beds, Resbeds, and the ratio of residents to physicians, Resdocs. We use the Resbeds variable to determine differences in teaching intensity, and the Resdocs variable to determine physician dedication to teaching residents (Campbell et al, 1991). Variables with a "1" are those for uncongested hospitals and those with "2" are congested.
There is a statistically significant difference between Ci(y,x) (the ratio of strongly disposable efficiency to weakly disposable efficiency) for hospitals with and without congestion) based on several tests, see Table 4. We also found a statistically significant difference between the hospitals without congestion and hospitals with congestion on measures of Residents per bed and Residents per physician (Resdocs1 for hospitals without congestion and Resdocs2 for hospitals without congestion). We also note that hospitals with congestion also had more residents per bed and residents per physician than hospitals without congestion, suggesting a direct relationship between the degree of congestion and teaching intensity. This result is supported by findings elsewhere in the literature that suggests residents have a negative impact on the productivity of other hospital staff (Jensen and Morrisey, 1986).
Table 4
One-sided Tests for Difference Between
Hospitals with Ci(y,x) = 1 and Ci(y,x) < 1
(Ho: mean or median of variables is equal)
t-test Mood Median X2 Kruskal Wallis H
Variables (p-value) (p-value)
(p-value)
Ci(y,x) 13.11 533 513
(0.000) (0.000) (0.000)
Resbeds -13.94 53.02 65.19
(0.000) (0.0001) (0.0001)
Resdocs -10.6 55.85 51.48
(0.000) (0.0001) (0.0001)
We also tested for differences by ownership form of the teaching hospitals and congestion. Table 5 indicates the frequency distribution between ownership and hospital congestion. We found a statistically significant Chi-Square of 26.731 which indicates that a relationship between ownership and congestion exists.
Table 5: Ownership and Hospital Congestion
Ownership Hospitals Without Congestion
Hospitals With Congestion
Public 49 36
Not-For-Profit 315 116
For-Profit 16 0
The small number of For-profit hospitals in the sample may be indicative of the fact that for-profit hospitals did not have a strong teaching commitment in the late 1980s as compared to not-for-profit hospitals and public hospitals. In order to determine if there was any difference in congestion by ownership type we examined the mean scores by ownership. These results are given in Table 6.
Table 6: Ownership and Hospital Congestion -- Descriptive Statistics
Ownership N Mean Congestion
Score Std. Dev.
Public 85 0.974 0.046
Not-for-Profit 431 0.994 0.023
For-Profit 16 0.9996 0.001
Public hospitals exhibited the most congestion on average and for-profit hospitals exhibited practically no congestion. Based on an F-test for the equality of these three means, we reject the null (F = 20.17, p-value = 0.000). We were not able to reject equality of means between not-for-profit and for-profit, however.
However, since we found that congestion was related to teaching intensity for the sample as a whole, we were also interested in the relationship between teaching intensity (in terms of resdocs) and ownership. These results are given in Table 7.
Table 7: Ownership and Teaching Intensity (Resdocs)
Ownership N Mean Std. Dev.
Public 85 .582 .405
Not-for-Profit 431 .186 .179
For-Profit 16 .078 .108
Differences among the three ownership forms were statistically significant in terms of teaching intensity. The F-test for equality of means of resdocs across the three ownership categories was F = 112.18, p-value = 0.000. The Mood and Kruskal-Wallis tests for equality of the median confirmed this result. In our sample public hospitals had the greatest teaching intensity and for-profit hospitals had the least, which may in part explain the low levels of congestion in the for-profit sector.
In summary, we found that medical residents did indeed >congest= the production of medical services in some teaching hospitals and differences exists among teaching hospitals that would lead to this result. In future research, we plan to compare the frontiers of teaching and non-teaching hospitals so that we provide further information regarding the resource costs for training medical personnel.
References
Cameron, James M. (1985) "The
Indirect Costs of Graduate Medical Education" New England
Journal of Medicine 312 (19), pps. 1233-1238.
Campbell, C. K., Gillespie, and J. Romeis (1991) "The Effects of Residency Training Programs on the Financial Performance of Veterans Affairs Medical Centers" Inquiry, 28, pps. 288-299.
Charnes, A; W. Cooper, and E. Rhodes
(1978) AMeasuring
the Efficiency of Decision-Making Units.@
European Journal of Operational Research, 3 (4), pps. 429-444
Fare R., S. Grosskopf, and C.A.K. Lovell (1986) The Measurement of Efficiency of
Production.
Boston: Kluwer Nighoff Publishing
Fare R., S. Grosskopf, and C.A.K. Lovell (1994) Production Frontiers New York:
Cambridge University Press
Farrell, M.J. (1957) AThe Measurement of Productive Efficiency. Journal of the Royal
Statistical Society,
Vol 120 (Part III), pps. 253-278.
Feinglass, J., J. Schroeder, GJ Martin,
W. Wallace, and J. Lyons (1991) "The Relationship of Residents'
Autonomy and Use of a Teaching Hospital's Resources" Academic
Medicine, 66 (9), pps. 549-552.
Grannemann, T., R. Brown, and M. Pauly
(1986) "Estimating Hospitals Costs: A Multiple Output Analysis"
Journal of Health Economics, 5, pps. 107-127.
Grosskopf, S.( 19860) AThe Role of the Reference Technology in Measuring Productive
Efficiency@
Economic Journal 96 (June), pps. 499-513
Lee, R. and J. Hadley (1985) "The
Demand for Residents" Journal of Health Economics
4, pps. 357-371.
Rich, EC, G. Gifford, M. Luxenberg,
and B. Dowd (1990) "The Relationship of House Staff Experience
to the Cost and Quality of Inpatient Care" Journal of
the American Medical Association 263 (7), pps. 953-957.
Rogowski, J. and J. Newhouse (1992)
"Estimating the Indirect Costs of Teaching" Journal
of Health Economics (11), pps. 153-171.
Rossmann, C. and K. Marcus (1990) "Uncertain
Medicare Payment Policy for Graduate Medical Education Costs"
Healthspan 7 (11) pps 11-17.
Steinwachs, D. "Redesign of Delivery
Systems to Enhance Productivity" (1992) Improving Health
Policy and Management, Editors: S. Shortell and U. Renhardt,
Ann Arbor, MI: Health Administration Press, pps. 275-310.
Sloan, F., R. Feldman, and B. Steinwald
(1983) "Effects of Teaching on Hospital Costs" Journal
of Health Economics 2, pps. 1-28.